Human Pancreas On a Chip To Identify CF-Related Diabetes
Scientists have created human pancreas on a chip which will enable the identification of the possible cause of a deadly and frequent complication of cystic fibrosis (CF) called CF-Related Diabetes, or CFRD.
It can be possible to also use the small two-chambered device, which features bioengineered human pancreatic organoids to study the causes of non-CF-related conditions such as type 1 and 2 diabetes, according to researchers at Cincinnati Children’s Hospital Medical Center. The study reports were published in Nature Communications.
For now, Scientists want to see if their device helps people with Cystic Fibrosis – CF a hereditary lung disease brought on by a mutation in the CFTR gene. The mutation leads to a salt and water strain on cell surfaces that clogs the lungs.
As individuals with CF get older, they become more at risk for CFRD, as per Anjaparavanda Naren, Ph.D., the study’s principal investigator and Director of the Cystic Fibrosis Research Center (Division of Pulmonary Medicine). Making things worse is that until now there has not been an efficient means to study CFRD in the laboratory to search for better remedies.
“Mouse models of CF do not faithfully recreate CF-Related Diabetes within the lab, and it wasn’t feasible to examine the disease in the depth we attained in this study,” said Naren. “Our technology closely resembles the pancreas and possibly may help us find curative measures to control glucose imbalance in people with CF, which is linked to increased illness and death.”
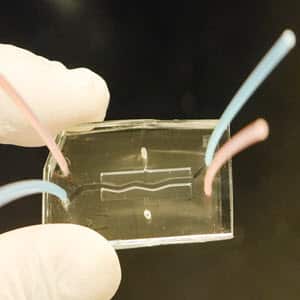
The in-vitro chip technologies may be employed to study CFRD and sugar imbalance in specific individuals with the condition, producing the potential for diagnosing different disease manifestations on a highly personalized basis. The chip will help assay variability in the glucose measures of different folks, determine the correlation of glucose levels with the CFTR mutation type, and test small-molecule interventions.
Cystic Fibrosis is known to cause by the CFTR gene but its exact role in CFRD is unclear. To answer this query, the investigators began by isolating pancreatic ductal epithelial cells and pancreatic islets given by patients.
The ductal organoids were in a transparent dual-chamber called a microfluidic device, which contained specific biochemical solutions to create the pancreas-on-a-chip. Ductal epithelial cells were cultured at the top chamber and pancreatic islet cells were at the bottom chamber, separated by a thin coating of a porous membrane that let the different chambers to interact.
The cells grew and expanded into three-dimensional pancreatic organs that mimicked cell-to-cell fluid and communications exchange, similar to the function of a naturally designed human embryo.
When the researchers tested pancreas-on-a-chip by disrupting CFTR gene expression, it impaired cell-to-cell communication, fluid exchange, and adversely affected endocrine function. This caused an insulin deficiency and recreated the CFRD disease procedure similar to that observed in the pancreas of a person. Researchers reported this confirmed the CFTR gene has a direct role in regulating insulin secretion and inducing diabetes in people with CF.
Devices have been around since 1979. But inventions in their layout and performance, especially since the advent of organoid engineering, now allow researchers to bioengineer human organ tissues and mimic the purpose of pure organs in a laboratory setting.
The research team, which includes study first author and research partner Kyu Shik Mun, PhD, will use the apparatus in a pilot study to examine FDA-approved drugs that modulate CFTR gene expression. The goal is to determine how well different CFTR drugs can reverse or slow lab-simulated CFRD.
Additionally, tinkering was co-corresponding study author Jamie Nathan, MD, surgical director of the Pancreas Care Center at Cincinnati Children’s.