3D Bio-printed Organ Breathes Fresh Air
Indeed a Eureka moment for all Bioengineers! A team of scientists has crossed a major hurdle on the path 3D printing replacement organs by discovering a breakthrough technique for bioprinting tissues. The innovation makes it possible for scientists to make entangled vascular networks that mimic the natural passageways for air, blood, lymph and other essential fluids of the human body.
The work was directed by bioengineers – Jordan Miller of Rice University, Kelly Stevens of the University of Washington along with 15 other collaborators from Rice, UW, Duke University, Rowan University and Nervous System, a design firm in Somerville, Massachusetts.
As per Miller, assistant professor of bioengineering at Rice’s Brown School of Engineering – Among the biggest roadblocks to creating functional tissue replacements is the inability to 3D print the complex vasculature that could supply nourishment to densely populated tissues. Technology discovered is one of the first of kind imprinting technology which addresses the challenge of multi vascularization in an immediate and thorough way.
Tissue engineering has struggled with this for a generation, said Stevens, assistant professor of bioengineering in the UW College of Engineering. This is an important matter, because how nicely a bioprinted tissue works will affect how effective it will be as a therapy.
The goal of bioprinting healthy, functional organs is driven by the demand for organ transplants. Over 100,000 individuals are on transplant waiting lists in the United States alone and those who do eventually receive donor organs face a life of immune-suppressing drugs to prevent organ rejection. Bioprinting has brought intense interest over the past decade since it could tackle both issues by enabling doctors to print replacement organs from an individual’s own cells. A ready supply of functional organs could be deployed to treat millions of patients worldwide.
“The liver is particularly interesting because it performs 500 different unique roles, likely second only to the brain,” Stevens said. “The liver’s sophistication means there is presently no machine or therapy that can replace all of its capabilities when it fails. Bioprinted human organs might someday supply that treatment.”
To deal with this challenge, the group created a new open-source imprinting technology known as the “stereolithography apparatus for tissue engineering,” or SLATE. The system employs manufacturing to make hydrogels that are gentle one layer at a time.
Layers are printed from a liquid pre-hydrogel solution that becomes a solid when exposed to light. With every layer, an overhead arm increases the gel to expose liquid into the next image. The insight by Bagrat and Miller Grigoryan, a Rice graduate student and lead co-author of this study, was the inclusion of food dyes that absorb light that is blue. The solidification is confined by these photoabsorbers to a layer that is fine. This way, soft, water-based gels can be produced by the machine with intricate internal architecture in a matter of minutes.
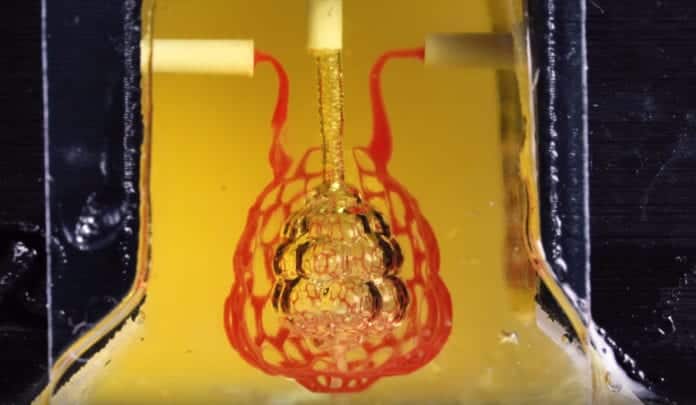
Tests of the lung-mimicking structure revealed that the tissues were sturdy enough to prevent exploding during blood circulation and pulsatile”breathing,” a rhythmic intake and outflow of atmosphere that mimicked the stresses and frequencies of human breathing. Tests found that red blood cells could take up oxygen as they flowed through a system of blood vessels surrounding the”breathing” air sac. This movement of oxygen is like the gas exchange that occurs in the alveolar air sacs of the lung.
To design the analysis most complicated lung-mimicking structure, which is featured on the cover of Science, Miller collaborated with research co-authors Jessica Rosenkrantz and Jesse Louis-Rosenberg, co-founders of Nervous System.
In the tests of therapeutic implants for liver disease, the team 3D printed cells, loaded them with primary liver cells and implanted them into mice. The cells had compartments for both liver cells and blood cells and have been implanted in mice with chronic liver injury. Tests showed that the implantation was lived by the liver cells.
Miller stated that all supply information in the experiments in the printed Science research is freely available. Additionally, all 3D files needed to build the stereolithography printing apparatus are available, as are for printing each of the hydrogels used in the 32, the design files. MHe added that his lab is using the new layout and imprinting methods to explore more complex structures.
“We’re just at the start of our exploration of the architectures found in the human body,” he explained. “We still have so much more to find out.”
Study co-authors include Rice’s Samantha Paulsen, Daniel Sazer, Alexander Zaita, Paul Greenfield, Nicholas Calafat, and Anderson Ta; UW’s Daniel Corbett, Chelsea Fortin, and Fredrik Johansson; Duke’s John Conley along with Amanda Randles; and Rowan’s Peter Galie.