Stem Cells May Help Restoring Sense of Smell – Tufts University Research
The sense of smell – it plays a vital role for all individuals. But all of that can be suppressed with aging, trauma, chronic sinus diseases, and neurodegenerative disorders. The inability or decreased ability to smell isn’t always treatable which is commonly called as called anosmia and hyposmia respectively in medical terms.
Tufts University School of Medicine Researchers has shown they can restore the sense of smell by developing and triggering olfactory stem cells in culture. They stated that this technique could be used to regenerate nose tissue, including sensory neurons.
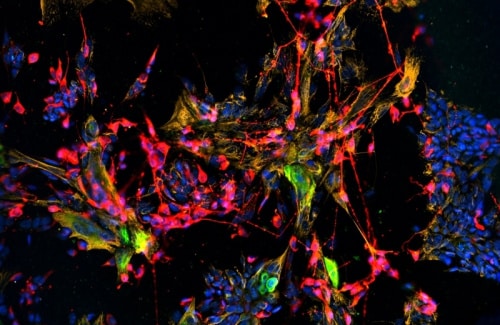
The olfactory epithelium has two kinds of stem cells namely globose basal cells (GBCs) and horizontal basal cells (HBCs) which is the sheet of tissue with neurons and supporting cells that line the nasal cavity. GBCs play the main role in the routine replenishment of nasal cells, and they’ve been successfully cultured. HBCs, on the other hand, remain dormant unless triggered by tissue injury. HBCs have proven difficult to keep in culture, limiting scientists’ ability to research them.
The lead was taken by the team from the conditions used to culture respiratory stem cells. From that point, they directed the stem cells to differentiate into olfactory epithelial cells like Sus cells, basal cells, and olfactory sensory nerves, before engrafting them into injured tissue.
In spite of the olfactory epithelium having a natural ability to regenerate serious injuries can trigger a permanent loss of smell. A 2016 NIH-backed study depending on the U.S. National Health and Nutrition Examination Survey found that smell dysfunction affects approximately 12.4percent of adults, which 3.2% of individuals have a complete or severe loss.
The team of tufts described how to culture HBCs in a study published in the journal Stem Cell Reports.
Director of Tufts Research James Schwob who is a professor of developmental, molecular and chemical biology with M.D and Ph.D. degree and who also led the group previously that showed a protein called p63 is a master regulator which was involved in the activation of HBCs. The Researchers found that lowering levels of p63 is necessary for HBC activation, so for this study, they further used retinoic acid to dial down levels of the protein.
Schwob stated that- Now that they can create a book of dormant stem cells, they see this as a helpful tool for investigating ways to direct cell differentiation toward particular cell types and develop new stem cell therapies for tissue and sensory regeneration or pharmacological interventions to activate the patient’s own dormant stem cells inside the nose.