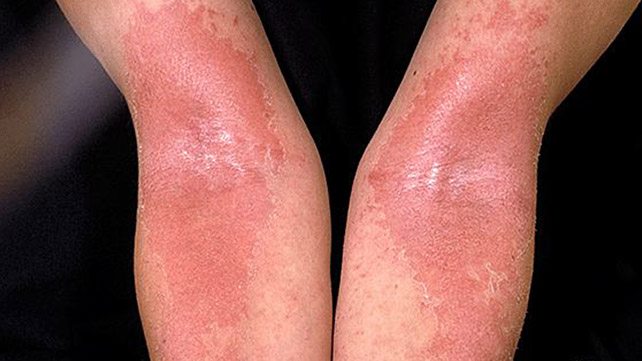
Skin’s Beneficial Bacteria Found to Help Alleviate Severity of Eczema
Atopic eczema aka atopic dermatitis is a chronic condition often developing in children before their first birthday; however, it may also develop for the first time in adults. Although found to improve significantly, or even clear completely, in some cases, it presently has no cure. Which is disturbing given how severe the condition is with it causing awfully itchy, dry, cracked, sore and red skin. And treatments currently aim at moisturizing and soothing the skin repair the skin barrier, in order to calm the itch and inflammation.
According to stats, approximately 12% of children in the US are diagnosed with atopic dermatitis every year. And the prevalence in the adult population—more than 10% according to a recent study—isn’t much different.
“Living with atopic dermatitis can be physically and emotionally challenging,” Anthony S. Fauci, director of the National Institute of Allergy and Infectious Diseases, said in a statement. “Currently available therapies can be time-consuming—requiring multiple daily applications—and costly.”
Despite the lack of clear evidence as to the cause of this inflammation, studies have previously suggested the skin microbiome—the community of bacteria and other microbes living on the skin—may play a key role. Furthermore, animal model studies at laboratory settings have discovered that a bacterium, Roseomonas mucosa, collected from healthy skin have qualities that might help assuage atopic dermatitis symptoms in patients.
Now, NIH scientists building on this evidence have designed an early stage clinical trial to test the safety and potential benefit of a treatment constituting R. mucosa for AD patients.
“By applying bacteria from a healthy source to the skin of people with atopic dermatitis, we aim to alter the skin microbiome in a way that will relieve symptoms and free people from the burden of constant treatment,” said NIAID’s Dr. Ian Myles, the study’s principal investigator.
The research involved collecting live Roseomonas mucosa bacterium from healthy individuals and applied to -10 adults and five pediatric eczema patients.
Twice weekly for six weeks, the adult participants were asked to spritz sugar water containing increasing amounts of this “good” skin bacterium onto their inner elbow and one other skin area of their choice. Additionally, these patients also underwent their regular eczema treatment. Kids in the study underwent a similar protocol for 12 weeks, after which the dose was upped to every other day for another four weeks.
After a few weeks, the team observed that the severity of the patients’ eczema/skin condition was reduced, and some participants even reported being able to cut back on steroid creams they’d used to treat their eczema.
No complications from the treatment were reported in the study. Overall, six of the 10 adults and four of the five children had over a 50 percent improvement in their AD symptoms by the end of the trial.
“By applying bacteria from a healthy source to the skin of people with atopic dermatitis, we aim to alter the skin microbiome in a way that will relieve symptoms and free people from the burden of constant treatment,” Myles says. “If future clinical studies demonstrate that this strategy is effective, we hope our work will lead to development of new, low-cost atopic dermatitis therapies that do not require daily application.”