Non-Invasive Device Allows WBC Levels Estimation in Chemo Patients
White-blood-cell (WBC) status is used as one indicator of immunological status in the diagnosis and treatment of multiple medical conditions, including cancer, infectious diseases, sepsis, autoimmune disorders, and in the use of immunosuppressant drugs.
However, all current methods require a blood sample which involves a visit to a healthcare center and trained clinical personnel, even with finger-prick technologies. This limitation inherently restricts how frequently and quickly monitoring can be performed.
MIT Bioengineers have now developed a noninvasive, portable device that could be used to monitor patients’ white blood cell levels at home, without taking blood samples.

The idea is to create a device that can be used to continuously monitor immunosuppressed patients, such as those on chemotherapy, and to detect serious infections.
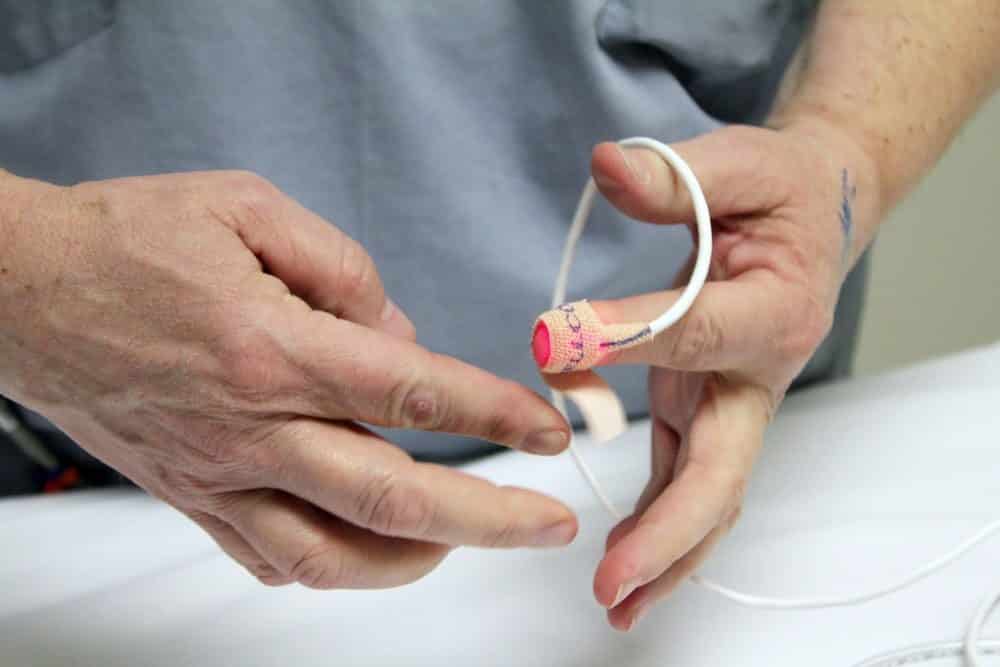
Their tabletop prototype records video of blood cells flowing through capillaries just below the surface of the skin at the base of the fingernail. A computer algorithm can analyze the images to determine if white blood cell levels are below the threshold that doctors consider dangerous.
“Our vision is that patients will have this portable device that they can take home, and they can monitor daily how they are reacting to the treatment. If they go below the threshold, then preventive treatment can be deployed,” says Carlos Castro-Gonzalez, a postdoc in MIT’s Research Laboratory of Electronics (RLE) and the leader of the research team.

The technology does not provide a precise count of white blood cells, but reveals whether patients are above or below the threshold considered dangerous — defined as 500 neutrophils (the most common type of white blood cell) per microliter of blood. The approach proved 95 percent accurate for determining whether a patient’s white cell levels were above or below the threshold when tested with 11 subjects at different points during their chemotherapy treatment.
“Based on the feature-set that our human raters identified, we are now developing an AI and machine-vision algorithm, with preliminary results that indicate the same accuracy as the raters,” says paper’s first author is Aurélien Bourquard, an RLE postdoc.

The research team has applied for patents on the technology and has launched a company called Leuko. To help move the technology further toward commercialization, the researchers are building a new automated prototype. Using this new prototype, the researchers plan to test the device with additional cancer patients. They are also investigating whether they can get accurate results with shorter lengths of video.
“There is a balancing act that oncologists must do,” says Sanchez-Ferro. “Normally doctors want to make chemotherapy as intensive as possible but without getting people too immunosuppressed. Current 21-day cycles are based on statistics of what most patients can take, but if you are ready early, then they can potentially bring you back early and that can translate into better survival.”