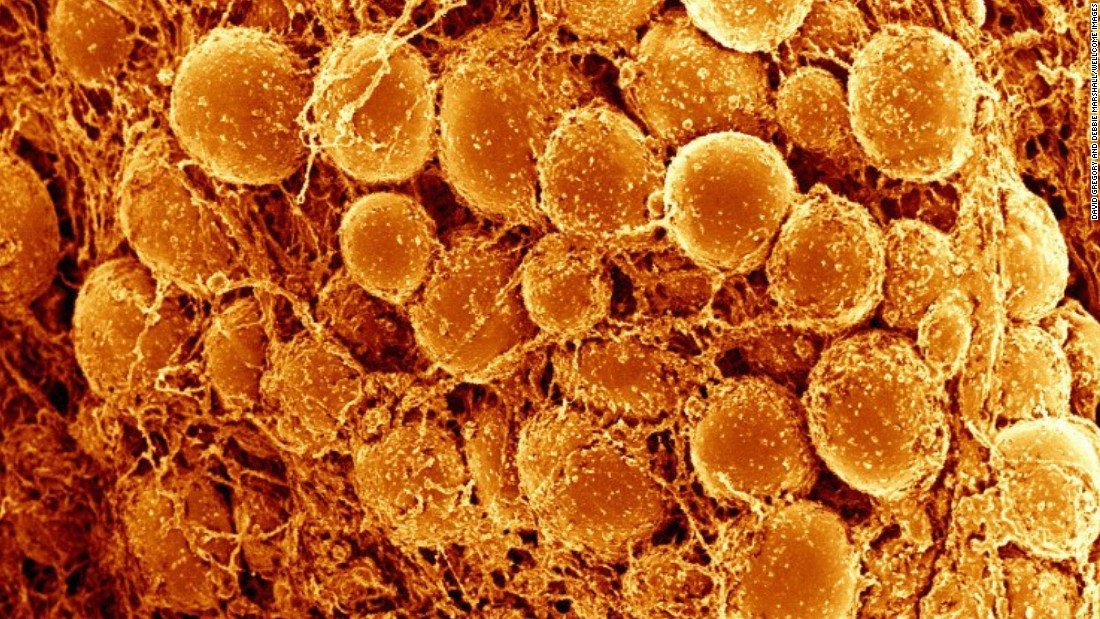
3D Imaging of Fat Cells Unveils Potential Targets to Fight Obesity
A team at The Rockefeller University‘s Laboratory of Molecular Metabolism has now adapted a revolutionary 3-D tissue imaging system called iDISCO that was originally designed to study the brain and used it to study “beige fat” in mice.
While the cell-intrinsic pathways governing beige adipocyte development and phenotype have been increasingly delineated, comparatively little is known about how beige adipocytes interact with other cell types in fat. This particular research builds on what is understood about the differences between the three kinds of animal fat: white, brown and beige fat.
White fat stores energy and hence has long been known to cause problems, but the brown and beige fat in contrast is believed to promote good health by burning energy. Beige fat in particular can be triggered to quickly switch from a dormant state to a highly active, energy-burning state.

“These findings highlight the value of 3D imaging as a discovery tool,” says graduate fellow Jingyi Chi, co-first author of the paper.
Chi and her colleagues, among them her co-first author Zhuhao Wu, wanted to know more about how beige fat cells interact with the sympathetic nervous system, which plays an important role in letting the cells know how much energy to store and how much to burn. However, conventional laboratory methods for looking at fat tissue (also known as adipose tissue) were insufficient—the images they produced lacked the necessary detail.
Therefore, through this adoption of the three-dimensional tissue imaging system known as iDISCO originally developed by another Rockefeller lab study, the team was able to look into mice that were exposed to the cold- which usually causes beige fat to develop and burn energy, they used the modified technology to visualize the internal architecture of the tissue.
Captured images were anything but bland- they provide a striking and unprecedented look at the functional features of beige fat, including blood vessels and projections from nerve cells that appear as filamentous networks. The presence and density of those nerve projections—both large nerve bundles and fine structures called neurites—predicted the activity level of the beige fat. The most active fat tissue had the most nerve projections. The 3D images also revealed important differences between visceral and subcutaneous fat.
Led by Paul Cohen, the team had previously demonstrated the importance of a protein known as PRDM16 in the creation and energy-burning activity of beige fat. Mice without the protein are unable to activate their beige fat and end up with many of the same complications that afflict obese humans, such as insulin resistance.
In order to determine the cause of nerve growth in the beige fat tissue and the role of PRDM16, the researchers studied subcutaneous fat tissue from mice that lack the protein in fat cells while exposing some of these animals to cold. The resulting images showed a “striking reduction” in neurite projections when compared to images from mice with the protein.
“This suggests that the two cell types engage in dialogue,” says Cohen, “where, if you have PRDM16 in a fat cell, it somehow guides the neurites to the site. And if you take it away, you don’t have those neurites.” It also suggests that the signaling molecules that mediate this dialogue could represent novel therapeutic targets in the ongoing battle against obesity and associated diseases.