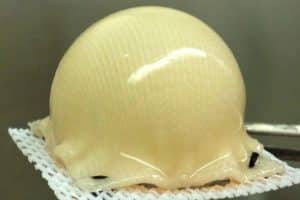
Genetically engineered hip-joint grown in lab from stem cells
With a goal of treating worn, arthritic hips without extensive surgery to replace them, scientists have programmed stem cells to grow new cartilage on a 3-D template shaped like the ball of a hip joint. What’s more, using gene therapy, they have activated the new cartilage to release anti-inflammatory molecules to fend off a return of arthritis.
The idea is to implant the perfectly shaped cartilage around the joint to extend its life before arthritis has caused too much damage to the bone.
Severe loss of cartilage can lead to bone rubbing on bone, altering the shape of the joint and forcing the bones out of their normal position.
The technology is likely to work for all joints, and could offer an alternative treatment for the 160,000 people in Britain who need hip or knee replacements each year, without the need for metal prosthetics.
“Replacing a failed prosthetic joint is a difficult surgery,” said Farshid Guilak, PhD, a professor of orthopedic surgery at Washington University. “We’ve developed a way to resurface an arthritic joint using a patient’s own stem cells to grow new cartilage, combined with gene therapy to release anti-inflammatory molecules to keep arthritis at bay. Our hope is to prevent, or at least delay, a standard metal and plastic prosthetic joint replacement.”
The technique uses a 3-D, biodegradable synthetic scaffold that Guilak and his team developed. The scaffold, molded into the precise shape of a patient’s joint, is covered with cartilage made from the patient’s own stem cells taken from fat beneath the skin. The scaffold then can be implanted onto the surface of an arthritic hip, for example. Resurfacing the hip joint with “living” tissue is designed to ease arthritis pain, and delay or even eliminate the need for joint-replacement surgery in some patients.
Additionally, by inserting a gene into the newly grown cartilage and activating it with a drug, the gene can orchestrate the release of anti-inflammatory molecules to fight a return of arthritis, which usually is what triggers such joint problems in the first place.
“When there is inflammation, we can give a patient a simple drug, which activates the gene we’ve implanted, to lower inflammation in the joint,” said Guilak, also a professor of developmental biology and of biomedical engineering. “We can stop giving the drug at any time, which turns off the gene.”
That gene therapy is important, he explained, because when levels of inflammatory molecules rise in a joint, the cartilage is destroyed and pain increases. By adding gene therapy to the stem cell and scaffold technique, Guilak and his colleagues believe it will be possible to coax patients’ joints to fend off arthritis and function better for a longer time.
The 3-D scaffold is built using a weaving pattern that gives the device the structure and properties of normal cartilage. Franklin Moutos, PhD, vice president of technology development at Cytex, explained that the unique structure is the result of approximately 600 biodegradable fiber bundles woven together to create a high-performance fabric that can function like normal cartilage.
Because the implant is made from a patient’s own stem cells, there is no risk of rejection.
“The implants are strong enough to withstand loads up to 10 times a patient’s body weight, which is typically what our joints must bear when we exercise,” said Dr Moutos.
The implants are currently being tested in laboratory animals and if all goes well, the team hopes to being human testing within three to five years.
Dr Bradley Estes, vice president of research and development at Cytex, added: “We envision in the future that this population of younger patients may be ideal candidates for this type of biological joint replacement.”
The research was published in the Proceedings of the National Academy of Sciences.